IT’S JUST A HEADACHE…I CAN DEAL WITH IT
Most of the people who read this will have suffered a headache, in one form or another, at some point in their lives. And for those of you who deal with headaches on a monthly, weekly, or perhaps even daily basis – I will be the first to come forward and say – “I get it”.
It was probably about 10 years ago when I started to get headaches more and more frequently. My headaches were never extremely severe or debilitating but more of a nuisance because they would stick around all day, every day and sometimes last up to two weeks. The most annoying part was that nothing seemed to help. I tried to brush it off and deal with my headaches for a couple years, always thinking to myself – “Oh, they’re probably just because I’m a typical student who is always tired from countless hours of studying and staring at either a textbook or computer screen”. I would always have a stash of Advil in my backpack – ready to try and knock that headache down a notch so it didn’t interfere too much with whatever I had on my agenda for the day. I never experienced much relief from the Advil or other anti-inflammatory pain relievers, but I didn’t know what else to do.
Eventually I became so fed up with my headaches, I started to explore other treatment options. I visited my family doctor (was referred for an MRI – no abnormal findings), checked in with my dentist (got a custom night guard because apparently I clench my teeth at night, which may have been contributing) and made a stop at the optometrist (got glasses with a minimal prescription in one lens, hoping that it MIGHT help decrease some strain on my eyes). After all this, still not much seemed to change.
My next resort was, you guessed it, a physiotherapist. I had never thought of going to a physiotherapist before, especially for treatment of my headaches, but I was willing to try anything. At this point, I was still an undergraduate student and was quite unfamiliar to the world of physio and what it had to offer – but little did I know, there is a lot of research out there to support how physiotherapy treatments can help manage different types of headaches (yes, there are different types of headaches!)
Having worked in a physiotherapy setting for a few years and now being a Physiotherapy Student at the University of Alberta, I’ve tried several treatment methods including neck mobilizations/manipulations, modalities, soft tissue/trigger point release and both acupuncture and IMS (Intramuscular Stimulation). All of these I will expand on below as I provide a quick and simple breakdown of the types of headaches, self-management of the symptoms and what PT treatment can do to help you!
HEADACHES & HOW PHYSIOTHERAPY CAN HELP
Even though the majority of the population gets headaches at one time or another, most don’t realize that there are different types of headaches that can be associated with different causes. The most common type of headache and one that generally responds well to physiotherapy treatment is called a cervicogenic headache.
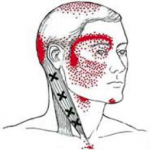
Stiff joints in the upper neck are the primary cause of cervicogenic headaches. Under ideal circumstances, joints are allowed to glide freely to provide pain-free movement of the neck. If a joint, surrounding ligaments or muscles are injured or irritated, the joints can become stiff and cause pain to be referred into areas of the head or around the eyes. Here is a list of symptoms that are generally associated with this type of headache:
- Constant and dull ache
- Slow onset with an unclear cause
- May be present for days, weeks or even months
- Stiffness or restricted movement of the neck
- Pain is worse on one side
- Pain radiates from the back to the front of the head
- Headache can be eased when pressure is applied at the base of the skull
- Headache worsened by sustained postures or certain neck movements
- Possible dizziness, light-headedness or nausea
Now to the big question, what can physiotherapy do to help? Physiotherapists can help address some of the key contributing factors to the development of cervicogenic headaches. The major contributing factors include:
- Poor posture
- Stiffness of the joints in the neck and upper back
- Muscle imbalances (muscle tightness + muscle weakness)
- Previous neck trauma (ex: whiplash, sports injury)
In order to properly tackle some of these factors, a full assessment of the neck and upper back is always carried out to provide an accurate focus for the treatment. Some of the treatment methods may include:
- Joint Mobilizations:
- Passive movement techniques that aim to restore full pain-free joint range of motion and overall movement of the neck
- Stretching:
- A regular stretching program is key in maintaining the flexibility of the neck muscles, which helps maximize function
- Strengthening:
- Ongoing neck problems are often linked with weakness of the postural and supporting neck/back muscles (chin poke + rounded shoulders = weak postural muscles)
- Massage/Trigger Point Release:
- Shortened muscles often have “trigger points” that can contribute to referred pain, relaxation or release of these tightened areas can help improve neck muscle function
- Modalities:
- Heat, TENS, IFC (Interferential Current) or EMS (Electrical Muscle Stimulation) can often be used in conjunction with manual techniques to help relieve some pain and muscle tension
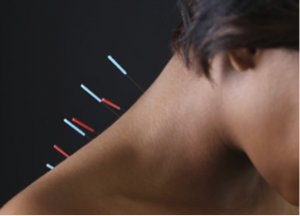
- Needling (Acupuncture or IMS):
- Acupuncture involves insertion of tiny needles to stimulate specific points near the surface of the skin in order to help restore blood flow and alter many conditions
- IMS (Intramuscular Stimulation) involves the same needles but follows completely different concept. The needles are inserted directly into a muscle to help relieve any muscle tension that could be irritating surrounding joints or nerves
A FEW TIPS TO HELP MANAGE HEADACHES ON YOUR OWN
- Improve your posture while standing & sitting at work, home and even while driving
- Sit/stand up straight
- Pull the shoulders back and down
- Tuck your chin back slightly
- Tuck your belly in
- Stretch out those muscles!
- Stretches should be held for AT LEAST 30 seconds (a minute is even better) and done several times throughout the day
- Do not hold your breath during stretches, allow your body to relax and breathe normally
- Go just far enough so that you feel a stretch…no pain
- Keep hydrated!
- Attempt to better manage your own daily stresses…easier said than done, I know.
Just remember, if you’re experiencing headaches, you shouldn’t have to just “deal with it”. Hopefully we can help!
Kelsea Bain, MScPT Student
References/Resources:
- 1. Magee, D.J., (2008). Orthopedic physical assessment (5th ed.). St. Louis, MO: Saunders Elsevier.
- 2. http://www.balmainsportsmed.com.au/index.php/injury-library/97-headaches-a-how-physiotherapy-can-help
- 3. http://www.physio-pedia.com/Cervicogenic_Headache
- 4. http://www.physioadvisor.com.au/9273650/cervicogenic-headache-neck-headache-physioadvi.htm