Picture this: You’re playing your favorite sport; and in the middle of the action, you take a wrong step. You “pop” your shoulder out of its place. You get wheeled off to the ER. The doctor fixes you up and tells you that you’re now good to go. Have you ever thought “okay, I’ve been told I’m good, now what?”, and “Will it be just like nothing ever happened”? In this blog topic, I’m going to talk about the ins and outs when it comes to shoulder dislocation.
What is the shoulder joint?
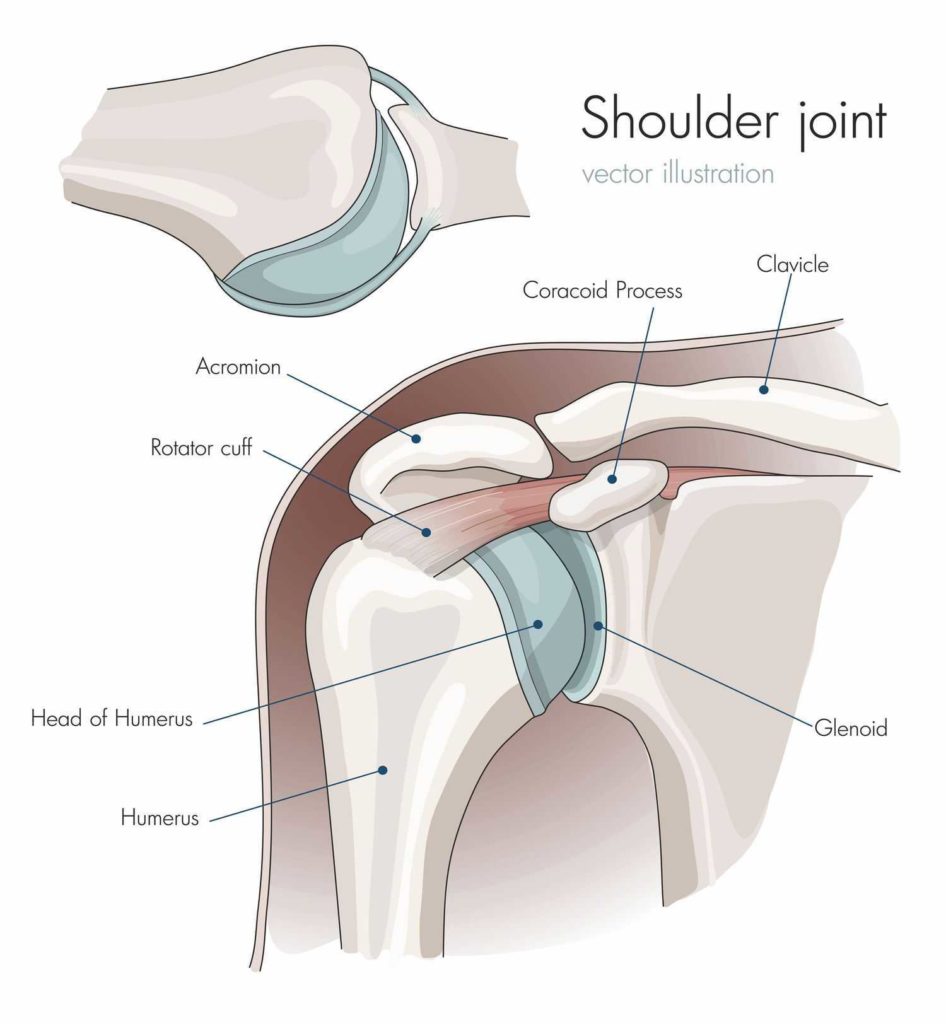
Before we begin, it’s good to have a general idea of what composes the shoulder joint and how it relates to its movements. The shoulder is a ball-and-socket joint, which consists of the humeral head (the ball), the glenoid (the socket) and the scapula (the shoulder blade where the socket attaches to). These structures are held in place by a series of ligaments, soft tissue and muscles, which act as movers and stabilizers for the joint.
Dislocation vs subluxation
When talking about “dislocation”, it’s important to distinguish between dislocation and subluxation. Both are instances wherein the ball is forced out of the socket, but the main difference is that in a dislocation, the structures stabilizing the joint are compromised. A subluxed joint only involves excessive movement, but without injury. A dislocated shoulder needs to be relocated by a medical professional. Once that’s done, the fun part now begins, rehabilitation!
Recovery
Now, how does this all tie back to “now what”? During rehabilitation, the first step is to find out which of the structures are affected most by the injury. The shoulder is a very mobile joint, and every movement will involve a muscle, or multiple muscles. In addition to muscles, we also verify if the ligaments, which help to hold the shoulder in place, and other soft tissues are in working order. Like a mechanic running tests on your car to see what’s causing those weird noises, we would go through a series of movements that tests every muscle that moves the shoulder. If a certain movement causes pain, that helps pinpoint which structure needs the most amount of rehabilitation. Typically, the rehabilitation process is split into three phases.
Phase 1:
Pain can be a problem particularly in the first 2-3 weeks. Your doctor may give you a prescription to help with pain relief, or you can control the pain with basic painkillers. Also, you may benefit from putting an ice pack on the sore area for 10-15 minutes.
We will give you some gentle movements for the arm and highlight the importance of good upright posture with your shoulders back and chest up, as this will prevent problems with shoulder muscle balance in the future.
It is important during this stage that you avoid positions that could cause re-dislocation. The most important position to avoid is holding your arm out at 90 degrees to your side with the palm facing upwards, especially if a force is being applied.
Phase 2:
For this phase, improvement of range of motion and muscle strength, especially the rotator cuff is the main focus, to re-establish the muscle balance in the shoulder. We will identify any weakness in these muscles and give you specific and appropriate exercises to strengthen them.
Phase 3:
The goal of this phase is to make progress towards functional and sporting activities, by helping you regain the neuromuscular control of your shoulder. This is achieved by exercising the unstable shoulder in positions that challenge the shoulder stabilizers.
This also re-trains your proprioception, which is your body’s awareness of where a limb is in space. How does this work? Inside the shoulder joint, you have receptors which detects the position of the joint. These messages are then sent to the brain. When these receptors detect a situation of potential tissue damage, the muscles are caused to contract by the brain. This then causes the joint to move, so decreasing the mechanical stress on the surrounding areas.
During the last phase, we will give you exercises that are as similar as possible to the movements you do during your sporting activities.
Another thing we take into consideration, other than the type of injury, is if it has happened more than once. Depending on the number of times the injury occurred, and the age of the injury, recurring injuries have a great effect on how long it takes to rehabilitate the joint, and how much functionality can be restored. The chances of recurrence will depend on how well the structures heal. If you perform regular strengthening exercises, the structural support will be greatly increased, therefore increasing joint stability, and reducing the chance of re-injury.
If you have any questions or concerns about your shoulder, please contact us.
Danica Cheng
Physiotherapist at Pivotal Physiotherapy
Ask me a question
Book an appointment with Danica
