Lumbar Spine Osteoarthritis/ Degenerative Disc Disease
What is it?
Osteoarthritis (OA) is a form of arthritis that features the progressive damage and eventual break down of the articular cartilage that lines our joints7. Cartilage is a firm, rubber like tissue that covers the surfaces of joints that allows our bones to glide on one another. If the cartilage breaks down due to wear and tear it will start to deteriorate and the bones begin to rub together. This rubbing together can cause pain, stiffness and swelling.
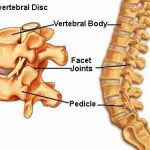
In the lumbar spine, the moving segments consist of the intervertebral discs as well as the facet joints (see picture above). Facet joints are the location where the vertebrae above and below touch each other. They carry approximately 20-25% of the spinal load when the intervertebral disc is intact5. With degenerative disc disease (DDD) the spinal load increases up to 70%5. This occurs because there is a reduction in the height of the disc, which increases the force on these facet joints. This leads to the loss of structural integrity that further strains the disc and causes a vicious cycle of deterioration2. There are three general stages that a person with DDD will experience. The first stage is significant dysfunction caused by acute low back pain. The second stage is the longest phase where there is relative instability at the degenerated segment7. The patient in this stage is susceptible to intermittent bouts of pain. The body re-stabilizing the segment characterizes the third stage and fewer episodes of back pain will occur7.
Without the proper management of degenerative disc disease, this condition may progress to more severe spinal pathologies such as stenosis, disc herniation or spondylolithesis.
Etiology (cause):
OA is most often atraumatic in nature, which means there was no specific trauma which caused the condition. OA usually occurs in individuals over the age of 50,5,6 and is commonly diagnosed through patient symptoms or diagnostic imaging8. However, it is emphasized that aging itself is not the sole cause of OA and should not be considered a part of ‘normal aging7. OA can result from a wide variety of conditions such as history of faulty posture, occupational tasks, prolonged immobilization, obesity, or repetitive mircotrauma.4, 7 Some evidence shows that there is a genetic component to osteoarthritis. Lower back pain is one of the most common reasons why adults seek medical attention, with 15-20% of adults reporting lower back pain each year9.
Signs & Symptoms:
It is important to understand that each individual who experiences back pain will present in a unique fashion. No two people will report the exact same symptoms. Some of the common signs and symptoms of degenerative disc disease are:
- Loss of range of motion (flexibility) 7
- Insidious onset (no distinct traumatic incident)5
- Pain usually with extension (but can occur with flexion)6,4
- Pain in low back and/or buttock5
- Commonly increased pain with standing, decreased pain with sitting5
Impairments:
- Reduced function in activities of daily living involving trunk mobility or prolonged or repetitive trunk motions (specifically activities requiring spinal extension) 4
- Impaired posture (forward flexion)4
- Pain with prolonged immobilization or excessive activity4
| What to avoid: | What to focus on: |
|
|
|
|
|
|
|
|
|
|
The focus of treatment:
Posture education and methods to manage pain are important aspects of this condition. Maintaining/ improving general cardiovascular fitness is important for patients with lumbar spine OA6. Examples of activities that will improve fitness and are important for our health are swimming, cycling (recumbent bike) or using an elliptical machine.
The importance of therapeutic exercises: What can physiotherapy do for you?
Seeking the proper medical advice and rehabilitation services will be critical in the management of this lifelong condition. Pursuing physiotherapy will help optimize your quality of life and prevent the development of a more severe spinal condition.
With lumbar spine osteoarthritis it is very common for pain to manifest in a cyclic pattern. This means that it is usual for back pain to feel good for a day but may perhaps be sore the next day. To break this cyclic pattern and to help decrease or manage the pain for the duration of your lifetime, physiotherapy will play an essential role. The physiotherapist will provide you with strategies to modify your daily tasks to enable you to perform them more easily. Time will be spent reviewing positions and postures to avoid, proper lifting techniques, proper postural positions as well as pain management strategies.
Physiotherapy for degenerative disc disease/ osteoarthritis will benefit you in many ways. There are a wide variety of evidence-based techniques that are currently being used to treat this common condition. A large focus of treatment will be on symptom and pain management. Modalities such as heat, ice, interferential current, ultrasound and transcutaneous electrical stimulation can be used where deemed appropriate. To help decrease pain and increase mobility of the spine, manual therapy becomes very important in managing this condition. Manual therapy consists of any hands-on treatment that the therapist may perform with you such as muscle mobilizations, stretching tight muscles, spinal mobilizations or manipulations.
Another large portion of physiotherapy treatment time will focus on providing you with exercises aimed to not only improve your symptoms but also to also maintain/ improve flexibility and increased the stability of the spine. Performing a regular exercise routine will help to reduce the severity and duration of any ‘flare-ups’. Moving the back in a controlled way helps promote the delivery of nutrients to the joints in the spine keeping the disc, muscles and ligaments healthier. Mechanical traction is a viable option and is worth discussing further with your physiotherapist.
Your physiotherapist will play an important role in managing this condition. Exercise compliance is the most critical component to anyone who suffers from lumbar osteoarthritis/ degenerative disc disease.
References:
- Chang, HJ. et. al. Osteoarthritis of the Lumbar Spine. Journal of the American Medical Association. 2010;304(1):114.
- Eliyas, J. & Karaholios, D. Surgery for degenerative lumbar spine disease. Di Mon. 2011;(57):592-606
- Fujiwara, A et al., The relationship between disc degeneration, facet joint osteoarthritis, and stability of the degenerative lumbar spine. Journal of Spinal Disorders. 2000;13(5):444-450.
- Kisner, C. & Colby, LA. Therapeutic Exercise – Foundations and Techniques. (5th ed) F.A. Davis Compnay, 2007.
- Magee DJ. Orthopedic Physical Assessment, 5th ed, Phil., WB Saunders, 2008.
- Magee, DJ, Zachazewski JE & Quillen WS. Pathology and Intervention in Musculoskeletal Rehabilitation. St Louis: Elsevier, 2008.
- O’Sullivan, SB, Schmitz, TJ. Physical Rehabilitation. (5th ed). F.A Davis Company, 2007.
- Raj, PP. Intervertebral disc: anatomy-physiology- pathophysiology-treatment. Pain Practice. 2008;8(1):18-44.
- Rubin, DI. Epidemiology and risk factors for spine pain. Neurology Clinical. 2007;25:353-71
